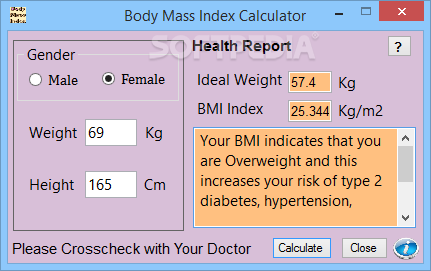
Medical News Today has strict sourcing guidelines and draws only from peer-reviewed studies, academic research institutions, and medical journals and associations. Doctors may use these variations when advising or treating conditions in specific people. The following table by the WHO shows some comparisons and cutoff points that may apply. The results of one 2011 study found that Asian American people within the healthy weight range were more likely to have symptoms of metabolic syndrome than their non-Hispanic white counterparts. In Korea, they added, there is evidence to suggest that almost twice as many people have features of metabolic obesity but a moderate weight compared with the United States. In 2017, Korean researchers pointed out that people in the Asia-Pacific region often have a higher risk of type 2 diabetes and cardiovascular disease at a BMI below the existing World Health Organization (WHO) cutoff point of 25 kg/m 2. They concluded that to predict obesity-type body fat percentage, the standard BMI threshold of 29.9 kilograms per square meter (kg/m 2) was appropriate for males but that a more suitable cutoff point for females appeared to be 24.9 kg/m 2. 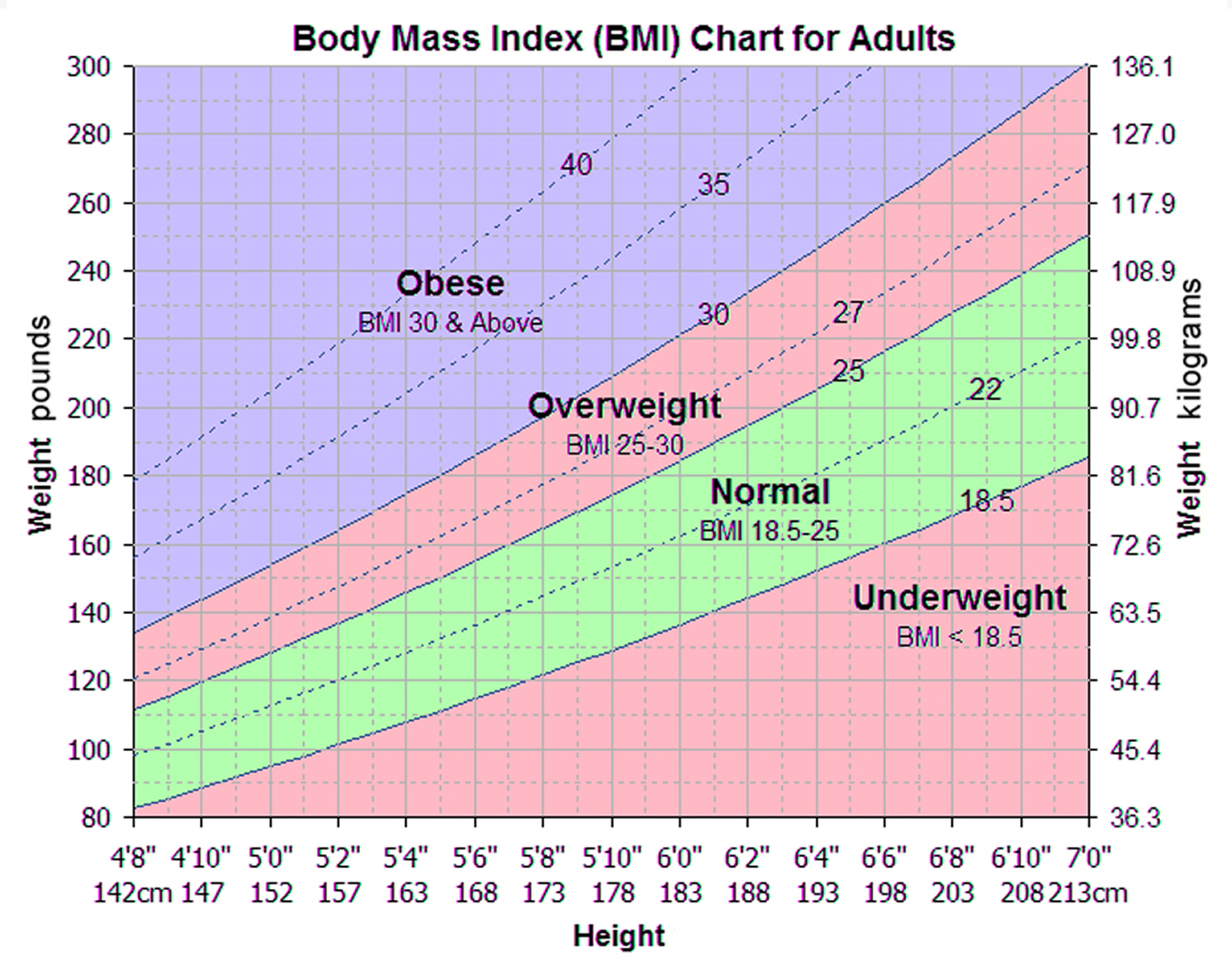
All rights reserved.Some evidence suggests that the associations between BMI, body fat percentage, and body fat distribution may differ across populations due to variations in sex, race, and ethnicity.Ī Brazilian study from 2017 looked at the correlation between BMI and body fat percentage in 856 adult males and females. Physiological explanations for these findings are discussed.Ĭopyright © 2016 Mayo Foundation for Medical Education and Research. The simple and inexpensive measure of BMI can be as clinically important as, or even more than, total adiposity measures assessed using accurate, complex, and expensive methods. We estimated Harrell's c-index as an indicator of discriminating/predictive ability of these models and observed that the c-index for models including BMI was significantly higher than that for models including BF% or FMI (P<.005 for all). When the analyses were restricted only to the sample assessed with hydrostatic weighing (N=29,959, 51.7%), the results were similar, with even slightly larger differences in favor of BMI (ie, HR, 3.0 95% CI, 2.2-4.0) compared with BF% and FMI (ie, HR, 1.5 95% CI, 1.2-1.9 and HR, 2.1 95% CI, 1.6-2.7, respectively). Compared with a medium FFMI, a very high FFMI was associated with an HR of 2.2 (95% CI, 1.7-2.7) for CVD mortality, with these estimates being markedly smaller for FFM (ie, HR, 1.2 95% CI, 0.9-1.6). For exact comparisons, the indices studied were categorized identically using sex-specific percentiles.Ĭompared with a medium BMI, a very high BMI was associated with a hazard ratio (HR) of 2.7 (95% CI, 2.1-3.3) for CVD mortality, which was a stronger association than for BF% or FMI (ie, HR, 1.6 95% CI, 1.3-1.9 and HR, 2.2 95% CI, 1.8-2.7, respectively). 
Body composition indices (ie, body fat percentage, fat mass index, fat-free mass, and FFM index ) were derived from either skinfold thicknesses or hydrostatic weighing. Body mass index was estimated using standard procedures. To examine whether an accurate measure (using a criterion standard method) of total body fat would be a better predictor of cardiovascular disease (CVD) mortality than body mass index (BMI).Ī total of 60,335 participants were examined between January 1, 1979, and December 31, 2003, and then followed-up for a mean follow-up period of 15.2 years.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
